Hereditary Gastrointestinal Cancer Genetic Diagnosis Laboratory – prevention of colon cancer in Hong Kong through genetic testing in high risk family
Doctor's Corner
What is Hereditary Colorectal Cancer?
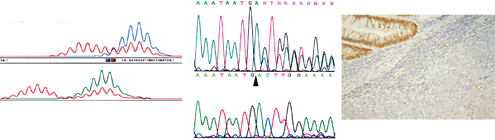
In Hong Kong, more than 4000 individuals develop cancer in the large bowel every year. The large bowel includes the colon and the rectum, and hence their cancers are called colorectal cancer. Although the exact cause of colorectal cancer is still unclear, most are caused by environmental factors and occur in individuals above the age of 50. However, about 5 – 10% of colon or rectal cancer are hereditary or familial, due to defects in the genes that can be passed on to offsprings. The two main types of hereditary colorectal cancers are the Lynch Syndrome (also known as Hereditary Non-polyposis Colorectal Cancer syndrome or HNPCC) and the Familial Adenomatous Polyposis (FAP) syndrome, which accounts for 4% and 1% of colorectal cancers respectively. Individuals affected by the Lynch (HNPCC) syndrome have no symptom until cancer develop. The most important clues to suspect HNPCC is occurrence of cancer in more than one family member, occurrence of multiple cancers in a single individual, and onset of the cancer at an early age. On the other hand, patients affected by the FAP syndrome are characterized by development of hundreds to thousands of precancerous (adenomatous) colorectal polyps. These polyps usually start to develop at the age of 16, and by age 40, one of these polyps may have evolved into colorectal cancer. The genetic defects causing these two syndromes are now known. HNPCC is caused by germline mutation in one of the DNA mismatch repair (MMR) gene. FAP is caused by germline mutation in the Adenomatous Polyposis Coli (APC) gene. It is important to note that for both types of familial colorectal cancer syndromes, cancer can be prevented by appropriate prophylactic screening or treatment. Thus, knowing whether you are affected by the disease can help you and your family members to take appropriate cancer prevention steps. Genetic diagnosis is now possible for affected patients and at risk family members. It can accurately identify individuals who carry mutation in the MMR or APC genes, and can distinguish amongst the family members who have inherited the mutated gene and who have not. For family members who have not inherited the mutation, they can be relieved of the psychological burden. For family members who have inherited the mutation, they can take appropriate cancer prevention steps.
Genetic Diagnosis Service and Research
The Hereditary Gastrointestinal Cancer Genetic Diagnosis Laboratory was established since 1995 and has been providing genetic diagnosis for families with familial colorectal cancer. This is a cancer prevention programme supported by the Hong Kong Cancer Fund. We are also actively performing research to understand the genetic basis of colorectal cancer. Using a state-of-the-art genetic diagnosis protocol catered for the Chinese population, we have successfully identified the causative germline MMR gene mutation for over 170 families with HNPCC syndrome, and performed genetic testing for over 800 family members. For the FAP syndrome, we have identified the causative germline mutation in over 80 families and performed genetic testing for over 350 family members. Our on-going research has shown a high incidence of early-onset colorectal cancer in Hong Kong, and a large proportion of these young patients with colorectal cancers in fact carry germline MMR gene mutation. We have identified a common founder mutation in Southern Chinese population, that originated from the Guangdong Province of China dating back to 550 to 2575 years ago. This founder mutation may accounts partly for the high incidence of early-onset colorectal cancer locally. We have also identified a new mechanism causing HNPCC, through deletion of the TACSTD1/EPCAM gene. The research data generated by our laboratory on the incidence and mutational spectrum of germline MMR gene mutation in our population and their association with early onset colorectal cancer has enabled us to formulate a rational strategy for genetic testing, management and prophylactic screening of young colorectal cancer patients and their family.
Who should undergo genetic testing?
HNPCC
If any of the followings are present in your family, you are at risk of HNPCC and
genetic testing may help you and your family.
- Early onset of colorectal cancer in an individual who is less than 50 years of age
- Two or more members in a family (first degree relatives) with colorectal or HNPCC-related tumors*, with one of the cancers being diagnosed under the age of 50
- Three or more members in a family with colorectal or HNPCC-related tumors*, regardless of age
- An individual who developed synchronous or metachronous colorectal, or other HNPCC-related tumors*, regardless of age
*HNPCC-related tumors
Cancers developing in the uterus, ovary, stomach, biliary tract, pancreas, small bowel, urinary tract, brain and skin.
FAP
For the FAP syndrome, if you or your family members are diagnosed with this disease, genetic testing can also help you.
Other Polyposis and cancer predisposition syndrome
We also provide genetic testing for the following syndromes:
Peutz-Jeghers Polyposis Syndrome, Juvenile Polyposis Syndrome, Cowden Syndrome, Li Fraumeni Syndrome, Hereditary Diffuse Gastric Cancer.
The Hereditary Gastrointestinal Cancer Genetic Diagnosis Laboratory of the Department of Pathology, The University of Hong Kong, Queen Mary Hospital is providing genetic diagnosis service for putative hereditary colorectal cancer patients. This is a cancer prevention programme supported by the Hong Kong Cancer Fund and is totally free of charge. We have set up a charitable patient referral centre named Hereditary Gastrointestinal Cancer Registry in St. Paul’s Hospital as a collaborative project. The Laboratory and the Registry together will provide appropriate genetic diagnosis, genetic counselling, psychosocial support and referral for prophylactic screening for patients in need. You can contact us to learn more about your family cancer pattern. A family tree will be developed to help us to assess your own cancer risk and that of your first-degree relatives. According to your family cancer pattern, we will provide appropriate genetic diagnosis tests and genetic counselling, in an attempt to identify the mutated gene responsible for your hereditary gastrointestinal tract cancer. This can then allow genetic diagnosis of your family members to determine who is a mutated gene carrier and who is not, and hence accurately predict their cancer risk. Based on the genetic diagnosis result, we can advice you and your relatives on appropriate preventive and screening measures and referral to appropriate health-care providers so as to achieve cancer prevention.
To learn more about HNPCC, click here.
To learn more about FAP, click here.
Publications from the Hereditary Gastrointestinal Cancer Registry Genetic Diagnosis Laboratory
- Yuen ST, Chung LP, Leung SY, Luk ISC, Chan SY, Ho JCI, Ho JWC, Wyllie AH. Colorectal carcinoma in Hong Kong: epidemiology and genetic mutation. Br J Cancer 1997; 76(12): 1610-1616.
- Leung SY, Chan TL, Chung LP, Chan ASY, Fan YW, Hung KN, Kwong WK, Ho JWC and. Yuen ST. Microsatellite instability and mismatch repair gene mutations in glioma. Am J Pathol. 1998; 153(4):1181-8.
- Chan TL, Yuen ST, Chung LP, Ho JWC, Kwan KYM, Chan ASY, Ho JCY, Leung SY, Wyllie AH. Frequent microsatellite instability and mismatch repair gene mutations in young Chinese patients with colorectal cancer. J Natl Cancer Inst 1999; 91:1221-1226.
- Chan TL, Yuen ST, Chung LP, Ho JWC, Kwan KYM, Fan YW, Chan ASY, Leung SY. Germline hMSH2 and differential somatic mutations in patients with Turcot’s syndrome. Genes Chromosomes & Cancer 1999; 25:75-81.
- Leung SY, Yuen ST, Chan TL, Chan ASY, Ho JWC, Fan YW, Hung KN, Chung LP and Wyllie AH. Chromosomal instability and p53 inactivation are required for genesis of glioblastoma but not for colorectal cancer in patients with germline mismatch repair gene mutation. Oncogene. 2000;19(35):4079-83.
- Ho JWC, Yuen ST, Chung LP, Kwan KYM, Chan TL, Leung SY, Chan ASY, Tse CW, Lam PWY and Luk ISC. Distinct clinical features associated with microsatellite instability in colorectal cancers of young patients. Int J Cancer. 2000; 89(4):356-60.
- Yuen ST. Colorectal cancer - Hereditary cancer syndromes and significance of genetic diagnosis. Hong Kong Society of Gastroenterology Newsletter. 2001 Jan; p.6.
- Chan TL, Yuen ST, Ho JWC, Chan ASY, Kwan KYM, Chung LP, Lam PWY, Tse CW and Leung SY. A novel germline 1.8-kb deletion of hMLH1 mimicking alternative splicing: A founder mutation in Chinese population. Oncogene 2001; 20(23):2976-81
- Yuen ST, Chan TL, Ho JW, Chan AS, Chung LP, Lam PW, Tse CW, Wylie AH, Leung SY. Germline, somatic and epigenetic events underlying mismatch repair deficiency in colorectal and HNPCC-related cancers. Oncogene 2002; 21(49):7585-7592
- Yuen ST, Davies H, Chan TL, Ho JW, Bignell GR, Cox C, Stephens P, Edkins S, Tsui WW, Chan AS, Futreal PA, Stratton MR, Wooster R, Leung SY. Similarity of the Phenotypic Patterns Associated with BRAF and KRAS Mutations in Colorectal Neoplasia. Cancer Res 2002; 62(22):6451-6455
- Chan TL, Chan YW, Ho JW, Chan C, Chan AS, Chan E, Lam PW, Tse CW, Lee KC, Lau CW, Gwi E, Leung SY, Yuen ST. MSH2 c.1452-1455delAATG is a founder mutation and an important cause of hereditary nonpolyposis colorectal cancer in the southern Chinese population. Am J Hum Genet. 2004; 74(5):1035-42
- Chan TL, Yuen ST, Kong CK, Chan YW, Chan AS, Ng WF, Tsui WY, Lo MW, Tam WY, Li VS, Leung SY. Heritable germline epimutation of MSH2 in a family with hereditary nonpolyposis colorectal cancer. Nat Genet 2006; 38:1178-83
- Ligtenberg MJ, Kuiper RP, Chan TL, Goossens M, Hebeda KM, Voorendt M, Lee TY, Bodmer D, Hoenselaar E, Brunner HG, van Kessel AG, Yuen ST, van Krieken HJ, Leung SY, Hoogerbrugge N. Heritable somatic methylation and inactivation of MSH2 in families with Lynch syndrome due to deletion of the 3’ exons of TACSTD1. Nat Genet 2009;41:112-117
- Thompson BA, Spurdle AB, Plazzer JP, Greenblatt MS, Akagi K, Al-Mulla F, Bapat B, Bernstein I, Capellá G, den Dunnen JT, du Sart D, Fabre A, Farrell MP, Farrington SM, Frayling IM, Frebourg T, Goldgar DE, Heinen CD, Holinski-Feder E, Kohonen-Corish M, Robinson KL, Leung SY, Martins A, Moller P, Morak M, Nystrom M, Peltomaki P, Pineda M, Qi M, Ramesar R, Rasmussen LJ, Royer-Pokora B, Scott RJ, Sijmons R, Tavtigian SV, Tops CM, Weber T, Wijnen J, Woods MO, Macrae F, Genuardi M, Castillejo A, Sexton A, Chan AK, Viel A, Blanco A, French A, Laner A, Wagner A, van den Ouweland A, Mensenkamp A, Payá A, Betz B, Redeker B, Smith B, Espenschied C, Cummings C, Engel C, Fornes C, Valenzuela C, Alenda C, Buchanan D, Barana D, Konstantinova D, Cairns D, Glaser E, Silva F, Lalloo F, Crucianelli F, Hogervorst F, Casey G, Tomlinson I, Blanco I, Villar IL, Garcia-Planells J, Bigler J, Shia J, Martinez-Lopez J, Gille JJ, Hopper J, Potter J, Soto JL, Kantelinen J, Ellis K, Mann K, Varesco L, Zhang L, Le Marchand L, Marafie MJ, Nordling M, Tibiletti MG, Kahan MA, Ligtenberg M, Clendenning M, Jenkins M, Speevak M, Digweed M, Kloor M, Hitchins M, Myers M, Aronson M, Valentin MD, Kutsche M, Parsons M, Walsh M, Kansikas M, Zahary MN, Pedroni M, Heider N, Poplawski N, Rahner N, Lindor NM, Sala P, Nan P, Propping P, Newcomb P, Sarin R, Haile R, Hofstra R, Ward R, Tricarico R, Bacares R, Young S, Chialina S, Kovalenko S, Gunawardena SR, Moreno S, Ho SL, Yuen ST, Thibodeau SN, Gallinger S, Burnett T, Teitsch T, Chan TL, Smyrk T, Cranston T, Psofaki V, Steinke-Lange V, Barbera VM. Application of a 5-tiered scheme for standardized classification of 2,360 unique mismatch repair gene variants in the InSiGHT locus-specific database. Nat Genet. 2014; 46(2):107-15.
If we can be of assistance or you have any further question, please contact our Coordinator:
Miss Dorothy Cheng
Hereditary Gastrointestinal Cancer Genetic Diagnosis Laboratory
Department of Pathology
The University of Hong Kong
Queen Mary Hospital,
Hong Kong
Tel: 28303729
Fax: 28949501
Email: colonreg@hku.hk
Web address: https://www.patho.hku.hk/en/colonreg
Directors of the Laboratory and the Registry
| Professor SY Leung Y.W. Kan Professor in Natural Sciences Chair Professor Department of Pathology The University of Hong Kong Queen Mary Hospital, Hong Kong |
Professor ST Yuen Consultant Department of Pathology St. Paul’s Hospital, Hong Kong and Honorary Clinical Professor Department of Pathology The University of Hong Kong, Hong Kong |